Florida, Minnesota
Pennsylvania, Tennessee
Welcome To the In-Pulse CPR Blog for News, Updates and Resources for the Medical Certification, Training and Health Industry
CPR, AED, First Aid, General Health & Medical News Blog
Topics…
American Heart 2025 guideline updates
Survival Stories – Featured
Why do we need First Aid training?
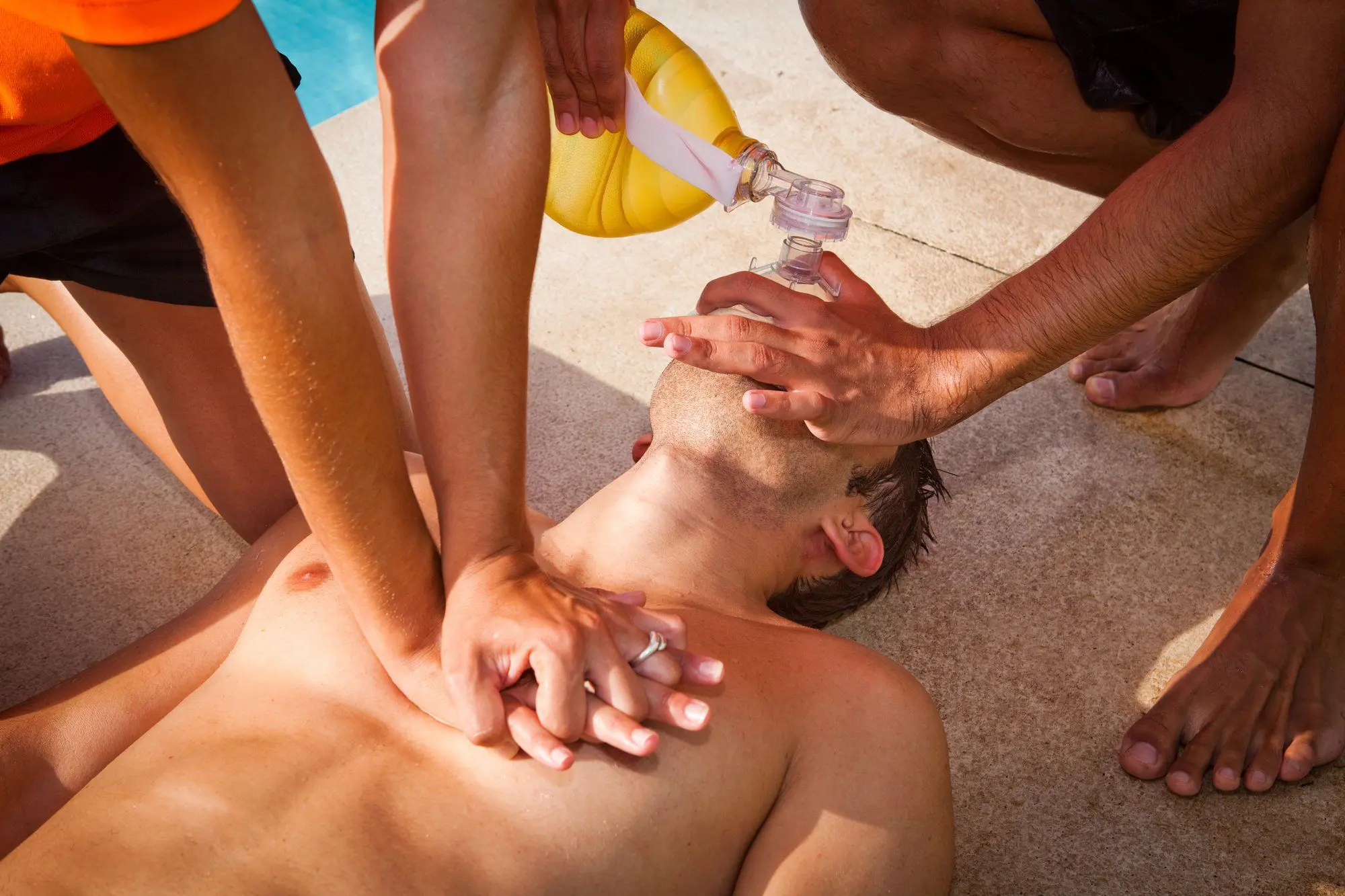


Blog Categories: What is CPR? | Why do we need CPR training? | Why do we need AED training? | Why do we need First Aid training? | Who needs Bloodborne Pathogens training? | What employers need to know about CPR training for their staff | Staying Healthy | Avoiding Injuries | Tributes to those who help make our lives safe | Survival stories | CNA Blog


