Nursing News: Passive Leg Raising and Elevating the Head during CPR Prove to Be Beneficial
Around 275,000 people, per year, experience OHCA (out-of-hospital cardiac arrest) incidents. This finding was reported by the National Center for Biotechnology Information (NCBI) in the U.S. National Institutes of Health’s National Library of Medicine archives. This number pertains to people living in Europe.
U.S. Statistics for OHCAs
It has also been found that a large number of people experience sudden cardiac arrest (SCA) in the U.S. or OHCAs. The number in the U.S. is even greater – about 365,000 per year. Of this number, around 90% end in death. This finding was recently published in the 2018 report, Heart Disease and Stroke Statistics, published by the American Heart Association (AHA).
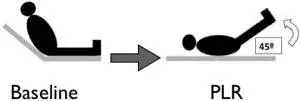
The Use of Passive Leg Raising (PLR). According to the NCBI report, the use of a passive leg raising (PLR) during cardiopulmonary resuscitation may assist in increasing the survival rates of OHCA victims. PLR during CPR has been shown to enhance cardiac preload and circulation when chest compressions are performed.
An Easy and Fast Technique
Like performing chest compressions, PLR is an easy and fast technique. Scientists have noted that the greatest benefit was experienced when PLR was performed during the early part of CPR, or prior to the first defibrillation.
Why PLR Works
A study designed to tests the use of PLR hypothetically concluded that elevation of the lower extremities during an OHCA CPR increases patient survival to one month by increasing cardiac preload and circulation to the bran and heart when chest compressions are performed.
Higher Neurological Scores
PLR may be of significant use when hands-only CPR is performed, or CPR that does not include the breaths associated with traditional CPR. One study also confirmed that using PLR during resuscitaiton resulted in higher neurological scores.
Increasing Survival CPR Rates
Cardiac arrest, itself, is a leading cause of death in both the U.S. and Europe. Therefore, any introduction of new techniques to increase survival rates is significant. Just as the name implies, a passive leg raise is a mechanical type maneuver the entails elevating the lower limbs from a horizontal position during resuscitation.
What Happens during PLR or Passive Leg Raising
During PLR, gravity causes the rechanneling of venous blood from the body’s lower extremities, which, in turn, triggers an increase in the left ventricular end-diastolic volume, carotid blood flow, right ventricular preload, and system venous return.
An Increase in Carbon Dioxide (CO2) Elimination
Based on these findings, researchers concluded that using PLR during CPR can improve survival rates. This information is important to nurses who are keeping up on the latest methods when applying CPR. Passive leg raising is useful when someone has fainted and has been shown to enhance carbon dioxide elimination when introduced in CPR.
Reviewing Past Reports
In fact, the first formal guidelines for CPR, introduced in 1974, included a statement that emphasized that at the “elevation of the lower extremities may . . . augment artificial circulation during . . . cardiac compression.” This statement was deleted from American Heart Association (AHA) guidelines in 1992. It is not included in the most recent guides either.
Measuring Chest Compressions
Clinical and preclinical studies support the American Heart Association’s recommendation that chest compressions should be at least 5 centimeters or 2 inches deep. When the chest is compressed too deep or at too fast of rate, the results can be adversely impacted.
The Importance of Maintaining Chest Compressions
Also, it is important to take note – interruptions during CPR, or chest compressions, can be harmful. Without compressing the chest, the blood flow can be negatively affected. In some instances, emergency or rescue personnel may stop chest compressions (in some cases, over a minute) to feel for a pulse, auscultate the chest, intubate or assess the underlying rhythm. Rescuers may forget, when hurried, to continue performing CPR.
Recent Statistics
One recent evaluation of CPR showed that these kinds of mistakes were indeed frequent and harmful. Nearly 50% of the time, compressions were inadequate, or performed at incorrect depths – all which did not fall in line with American Heart Association (AHA) guidelines.
Poorer Results
For instance, about 1/3 of the subjects received compressions at rate that surpassed 120 compressions per minute. When the compression rates were higher—or over the recommended 100 compressions per minutes—the results were poorer.
Maintaining the Proper Compression Rate – Why It Is Important
If the compression rate is too fast, the diastolic filling times may be insufficient and full recoil and compression depth may not be realized. A slight vacuum is created within the thorax during a passive chest recoil, which draws some of the blood back inside the heart and air into the lungs. Blood is then drawn from the extrathoracic to intrathoracic areas, where the heart is partially refilled until the completion of next compression.
Moreover, if a rescuer leans on the chest and prevents it from recoiling fully after a compression, the intrathoracic pressure will surpass the atmospheric pressure. When this happens, it reduces the refilling process in the heart and lowers the ICP (intracranial pressure). A full chest recoil maintains the ICP. To support this information, research with animals has demonstrated that leaning on the chest during resuscitation reduces the perfusion pressures to the myocardium and brain.
Errors Affect Survival Rates
In addition, compressing and decompressing at too fast of rate (over 120 compressions per minute) decreases the venous return time to less than what is needed for refilling the heart. Therefore, these kinds of errors can negatively affect survival rates. As a result, not only is imperative that nurses take CPR classes to learn the correct ways to perform hands-only and traditional CPR, it is essential that other advances be noted in resuscitation methods as well.
Elevating the Head during CPR
For instance, not only is passive leg raising an important consideration, so is learning about the position of the head during the lifesaving measure. For example, by convention, cardiopulmonary resuscitation has been performed for at least 50 years with the patient lying in a supine position. The entire body is positioned on the same plane, or horizontal on the floor.
Enhancing the Blood Flow
Recent research suggests that elevating the head during CPR has a marked beneficial effect on ICP (intracranial pressure) and brain circulation when compared to horizontal placement. When the body is supine and lies horizontal, each compression is related with the generation of waves resulting from arterial and venous pressure.
Increased Perfusion
If the patient’s head is elevated, the gravity drains the venous blood from the brain and sends it back to the heart. This results in increased refilling of the heart after compressions and a reduced compression phase ICP. As a result, studies show that elevating the head during CPR may offer more protection to the brain and increased perfusion or blood flow.
Supplementing Your Lifesaving Skills
Nurses can also get involved in learning methods to enhance post-resuscitation care. However, unless high-quality CPR is performed, these measures cannot be implemented with optimum effect. That is important to remember if you, as a nurse or other healthcare worker, want to supplement your lifesaving skills.
References:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4096750/
http://www.sca-aware.org/sca-news/aha-releases-latest-statistics-on-sudden-cardiac-arrest



