Proper precautions and training can prevent the spread of bloodborne pathogens
By Pearl Salkin, Updated 2026 by Val.
If a lab technician at a major medical research center drops a glass beaker, it’s highly unlikely that any bloodborne pathogen present will trigger a chain reaction leading to widespread infection. That’s not luck—it’s the result of strict safety protocols governed by the Occupational Safety and Health Administration (OSHA), designed to protect both workers and the public from biological hazards.
Bloodborne pathogens are infectious microorganisms found in human blood that can cause disease. When proper precautions are followed in environments where exposure is possible, the risk of transmission can be dramatically reduced—often nearly eliminated.
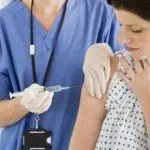
While HIV and AIDS have dominated headlines for decades, two other bloodborne pathogens pose significant and often underrecognized risks: hepatitis B (HBV) and hepatitis C (HCV). These viruses continue to spread across the U.S. and globally, often without the same level of public awareness.
The most effective way to control the spread of bloodborne pathogens is prevention at the source—especially in workplaces where exposure is possible. This starts with proper training for anyone who may come into contact with human blood. Employees must understand how to safely respond to incidents involving blood, which may carry infectious diseases.
OSHA has established guidelines and regulations, including the Needlestick Safety and Prevention Act, to address occupational exposure risks. These standards outline everything from minimizing exposure risks to responding appropriately when incidents—such as injuries involving contaminated sharps—occur.
Bloodborne Pathogen Requirements by State
| Requirement Area | Minnesota (MN) | Pennsylvania (PA) | Florida (FL) | Tennessee (TN) |
|---|---|---|---|---|
| Governing Standard | Federal OSHA adopted by MNOSHA | Federal OSHA | Federal OSHA | Federal OSHA |
| Core Regulation | OSHA 29 CFR 1910.1030 | OSHA 29 CFR 1910.1030 | OSHA 29 CFR 1910.1030 | OSHA 29 CFR 1910.1030 |
| Who Must Be Trained | Employees with occupational exposure to blood or OPIM | Same as federal OSHA | Same as federal OSHA | Same as federal OSHA |
| Training Frequency | Initial + annual refresher required | Initial + annual | Initial + annual | Initial + annual |
| Training Content Required | Exposure risks, PPE, transmission, emergency response | Same | Same | Same |
| Hepatitis B Vaccine | Must be offered within 10 days of job assignment | Same | Same | Same |
| Exposure Control Plan | Required (written plan) | Required | Required | Required |
| Post-Exposure Follow-Up | Required at no cost to employee | Same | Same | Same |
| Recordkeeping | Training + exposure records required | Same | Same | Same |
| State-Specific Additions | • Employee Right-to-Know (ERTK) law • Additional safety program (AWAIR) requirements | None beyond OSHA | None beyond OSHA | None beyond OSHA |
| Special Industry Rules | Body art requires 5 hours BBP training for licensing | Varies by licensing boards | Varies by licensing boards | Varies by licensing boards |

Certain professions clearly require this training, including healthcare workers, lab technicians, dental professionals, EMTs, and even tattoo artists. However, exposure risks extend beyond these roles. Employees in industries such as manufacturing, construction, warehousing, maintenance, and retail may also encounter situations involving blood, particularly during workplace injuries.
Even a well-intentioned coworker providing first aid for a minor cut can unknowingly be exposed. OSHA defines occupational exposure as reasonably anticipated contact with blood or other potentially infectious materials through the skin, eyes, mucous membranes, or by injury.
Because of this, relying solely on whether a workplace is mandated to follow bloodborne pathogen standards is not enough. Any organization where injuries could occur should consider comprehensive first aid and bloodborne pathogen training.
Preparing employees with the knowledge and tools to respond safely isn’t just about compliance—it’s about protecting people. In situations where seconds matter and risks are not always visible, proper training is one of the most practical and responsible investments a workplace can make.
Bloodborne Pathogen (BBP) Training – Who Needs It & How Often
| Industry / Role | Examples of Jobs | BBP Training Required? | How Often? | Why They’re at Risk |
|---|---|---|---|---|
| Healthcare | Doctors, Nurses, CNAs, Medical Assistants | ✅ Yes | Initial + Annual | Direct exposure to blood, needles, patient care |
| Dental | Dentists, Hygienists, Assistants | ✅ Yes | Initial + Annual | Oral procedures with blood exposure |
| Emergency Response | EMTs, Paramedics, Firefighters | ✅ Yes | Initial + Annual | Trauma response, bleeding injuries |
| Laboratories | Lab Techs, Phlebotomists | ✅ Yes | Initial + Annual | Handling blood samples |
| Hospital Support | Housekeeping, Laundry, Maintenance | ✅ Yes | Initial + Annual | Contact with contaminated materials |
| Tattoo / Body Art | Tattoo Artists, Piercers | ✅ Yes (often state required) | Initial + Annual (or per license) | Skin penetration, blood contact |
| First Responders (Non-Medical) | Police, Security Officers | ✅ Yes | Initial + Annual | Injury response situations |
| Schools & Childcare | Teachers, Daycare Staff, School Nurses | ✅ Yes (if first aid duties) | Initial + Annual | Assisting injured children |
| Coaches & Athletics | Coaches, Athletic Trainers | ✅ Yes | Initial + Annual | Sports injuries, bleeding |
| Janitorial / Custodial | Cleaning Staff, Custodians | ✅ Yes (if exposure possible) | Initial + Annual | Cleaning blood or bodily fluids |
| Funeral Services | Morticians, Embalmers | ✅ Yes | Initial + Annual | Handling human remains |
| Correctional Facilities | Guards, Staff | ✅ Yes | Initial + Annual | High-risk injury environment |
| Manufacturing / Industrial | Machine Operators, Line Workers | ⚠️ Often Required | Initial + Annual | Workplace injuries involving blood |
| Construction | Contractors, Laborers | ⚠️ Often Required | Initial + Annual | Cuts, trauma incidents |
| Warehousing / Logistics | Warehouse Staff, Forklift Operators | ⚠️ Often Required | Initial + Annual | Box cutters, equipment injuries |
| Automotive / Mechanics | Mechanics, Technicians | ⚠️ Sometimes Required | Initial + Annual | Injuries in shop environments |
| Food Processing / Butchers | Meat Cutters, Processing Workers | ⚠️ Often Required | Initial + Annual | Sharp tools, frequent cuts |
| Retail / General Workplace | Store Employees, Supervisors | ⚠️ Sometimes Required | Initial + Annual | First aid response to injuries |
| Maintenance / Facilities | Building Maintenance, Grounds Crew | ⚠️ Sometimes Required | Initial + Annual | Injury cleanup, sharp hazards |
| Hospitality | Hotel Staff, Housekeeping | ⚠️ Sometimes Required | Initial + Annual | Guest injury response, cleanup |
| Good Samaritan Employees | Any employee expected to provide first aid | ⚠️ Often Overlooked but Required | Initial + Annual | Assisting injured coworkers |



COMMENT (1)
Carol / December 27, 2011
I guess the best and most practical way to be prepared to handle an incident is to wear gloves if you know you there is a possibility of coming in contact with with bodily fluids/blood. Even if you wear gloves, it is important that you wash your hands after proper removal of the gloves. Not sure, how to do that? Sign up for a first aid class (any AHA first aid class) will make certain you know how to properly remove gloves. Seems simple, but it is so important.