The Role of CPR Training in Enhancing Workplace Safety
Having a safe and secure workplace is one of the most important responsibilities of any business owner or manager. It is essential to ensure that everyone in the workplace is aware of and trained in the proper safety protocols and procedures. One of the most important safety protocols is CPR training. This lifesaving skill can be the difference between life and death in an emergency. At In-Pulse CPR, we provide private group training in Florida, Pennsylvania, and Minnesota to ensure your team is prepared together. Check our course schedule in your state and keep reading to learn more about the role of CPR training in improving workplace safety.
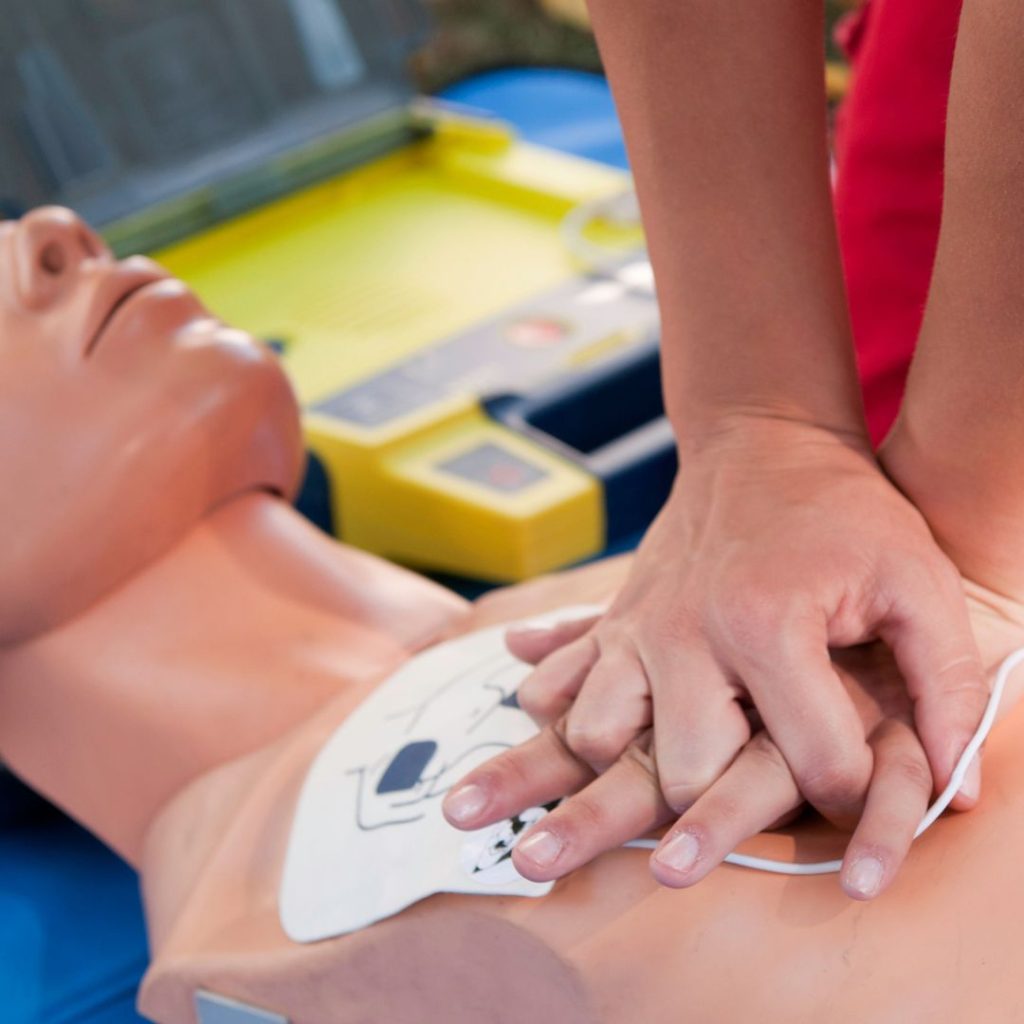
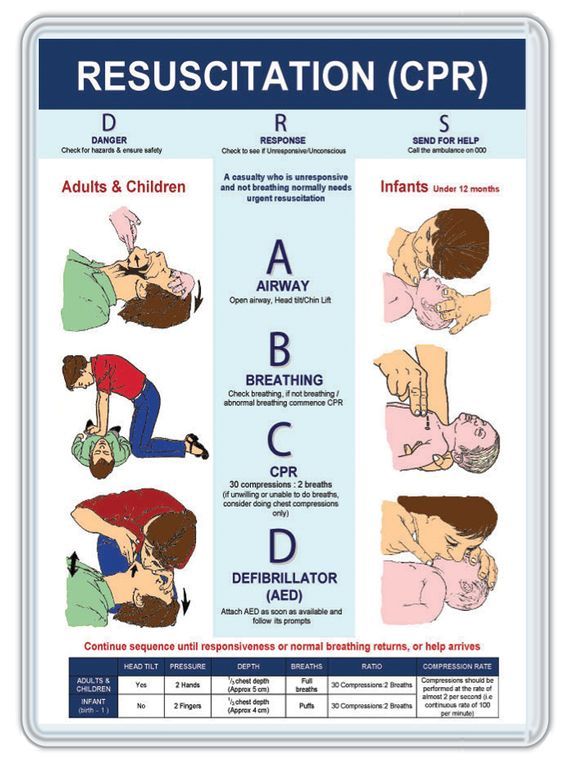
The Importance of CPR Training
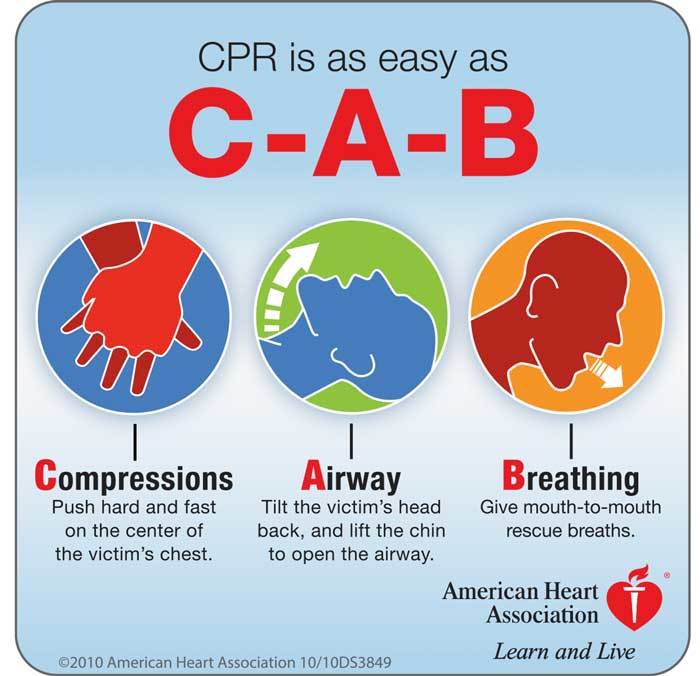
CPR training is a critical safety protocol that can be the difference between life and death in an emergency. When done correctly, CPR can help save lives and limit the amount of damage caused by a medical emergency. It is important to have CPR training in the workplace as it will increase the chances of survival if an emergency situation arises.

Benefits of Group Training
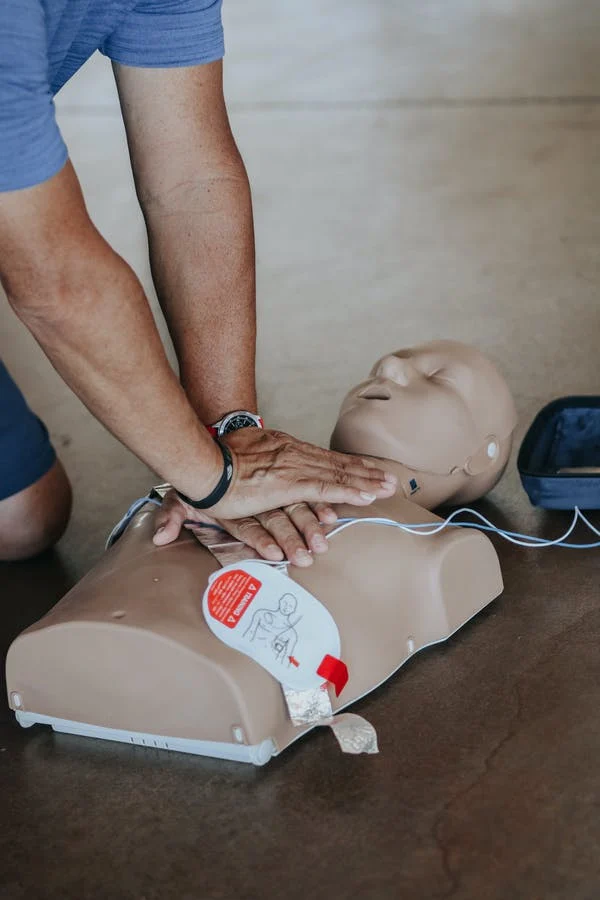
Group training is a great option for businesses looking to ensure that their team is prepared for any emergency situation. It is an effective way to teach multiple people at once, and it also allows for an engaging and interactive learning experience. Group CPR training also provides an opportunity for the group to practice their skills together, which can be especially beneficial in an emergency.
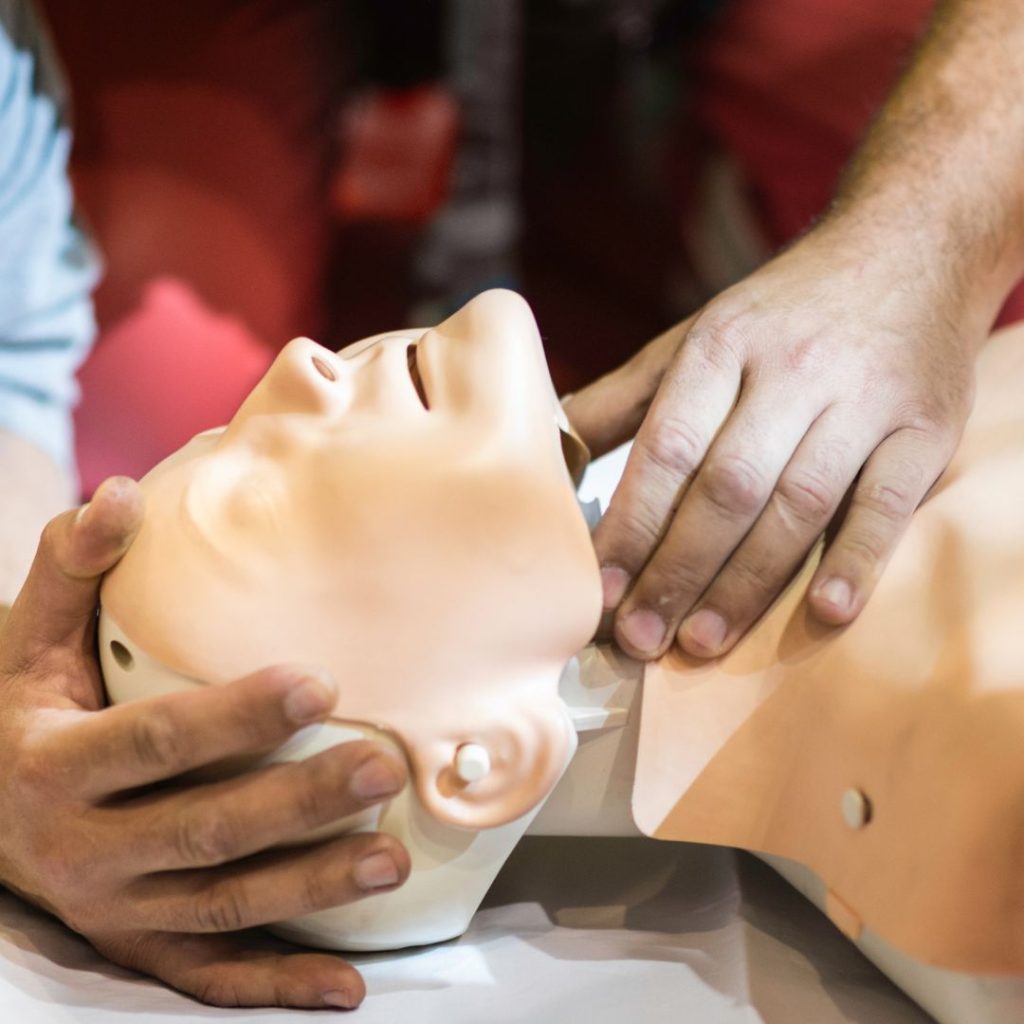
In-Pulse CPR Courses
At In-Pulse CPR, we provide private group trainings that are a great way to have your team prepared together. Our courses are hands-on, engaging, and interactive and offer the opportunity for the group to practice together. We offer CPR training in Florida, Pennsylvania, and Minnesota, making it easy for businesses in those states to take advantage of our services.
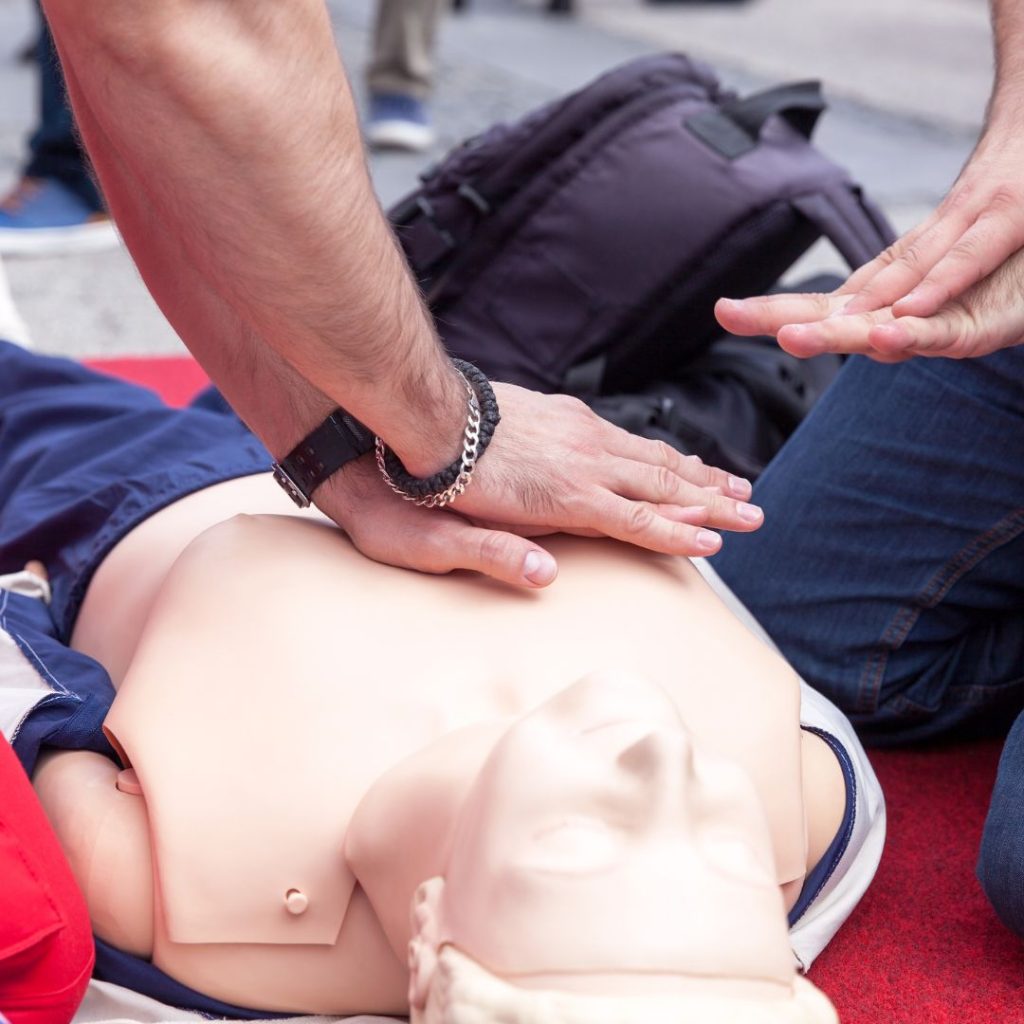
Get Prepared
CPR training is an invaluable asset to any workplace safety program. Having your team trained in CPR can help keep your workplace safe and provide peace of mind in the event of an emergency. In-Pulse CPR’s private group trainings are a great way to get your team prepared together.
By taking the necessary steps to keep your workplace safe, you are showing that you care about the safety of your team and that you are committed to providing the best possible environment for them. Our private group training at In-Pulse CPR is a great way for your team to become prepared, learn, and practice together. Contact us today to learn more about our CPR training courses in Florida, Pennsylvania, and Minnesota.