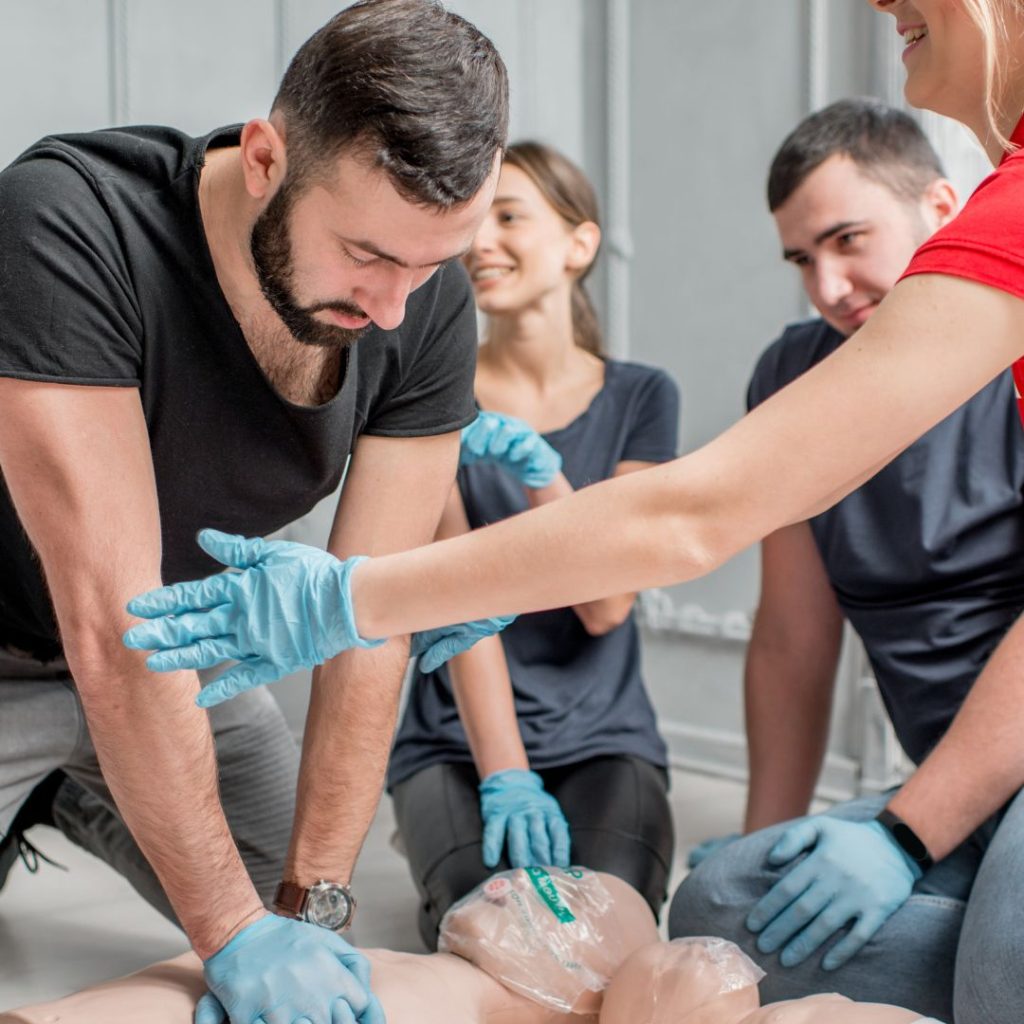
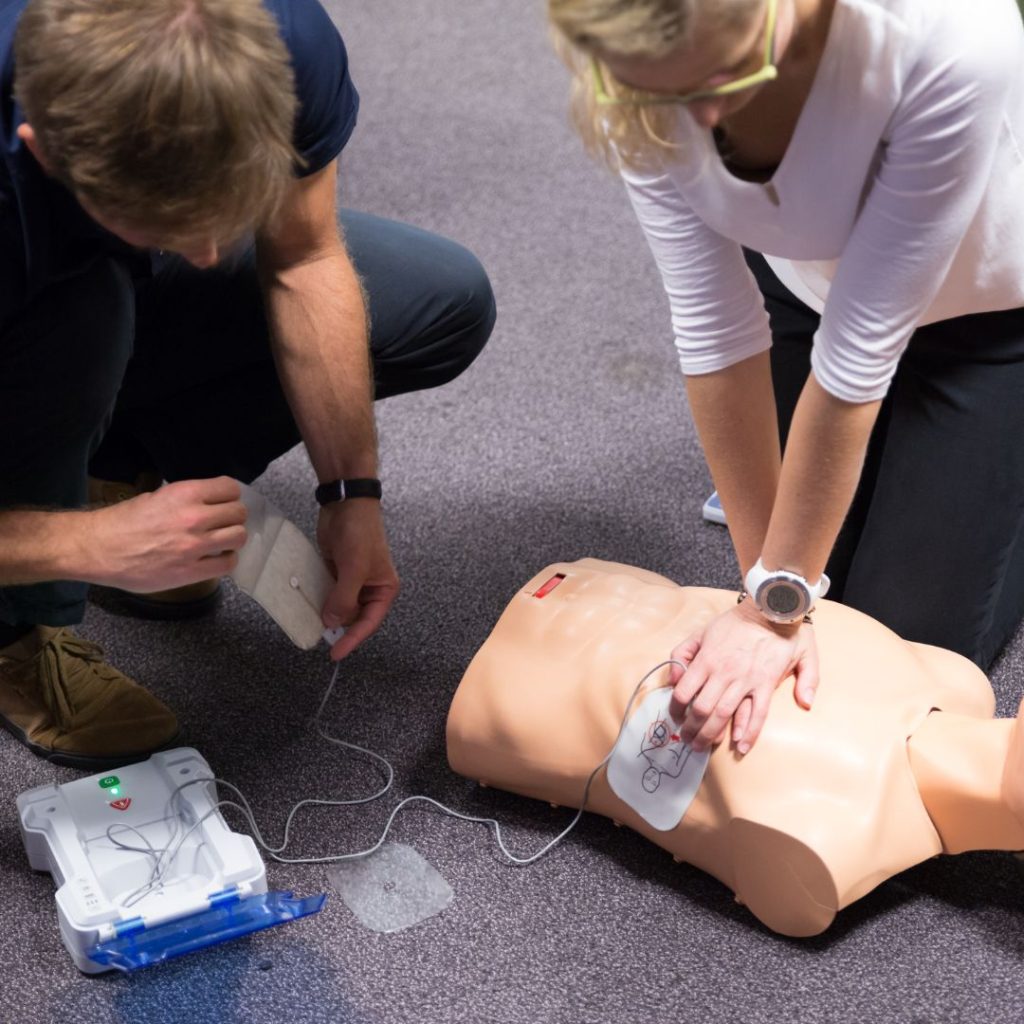
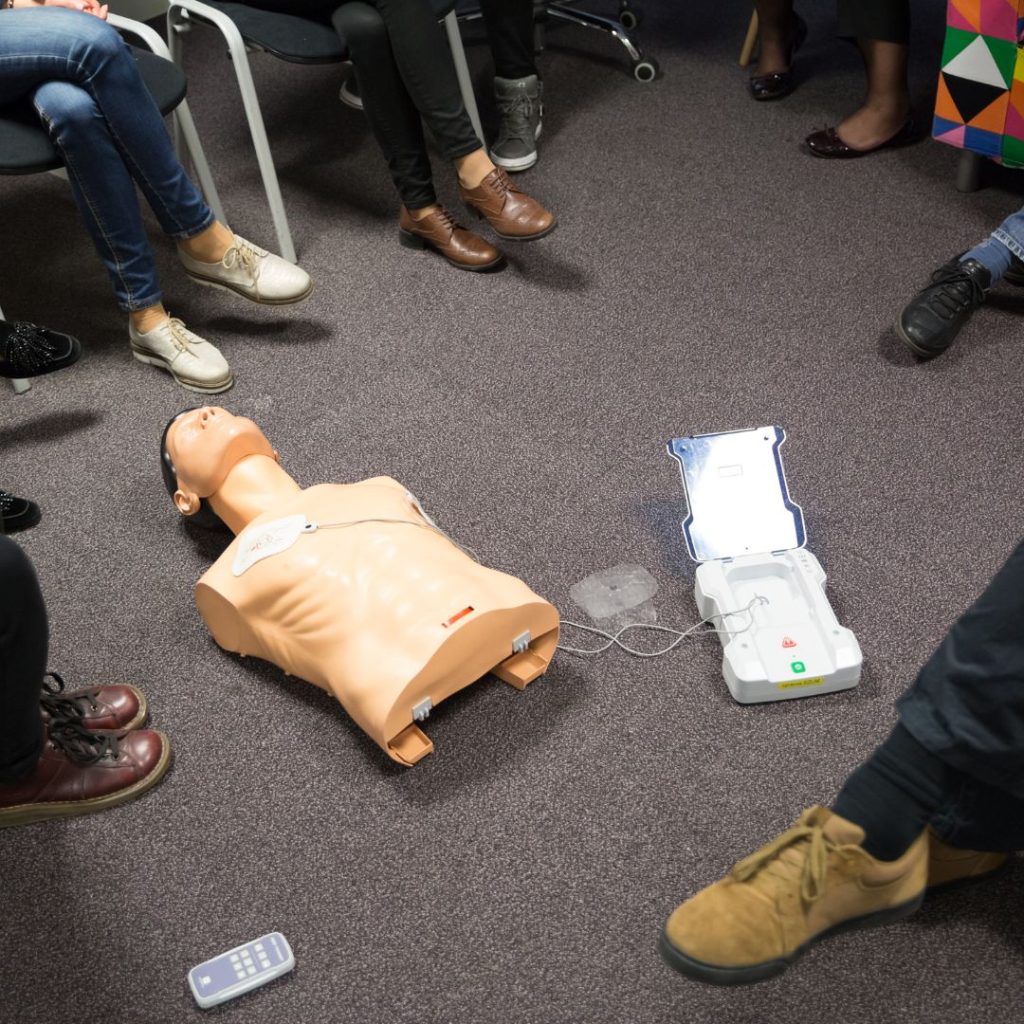
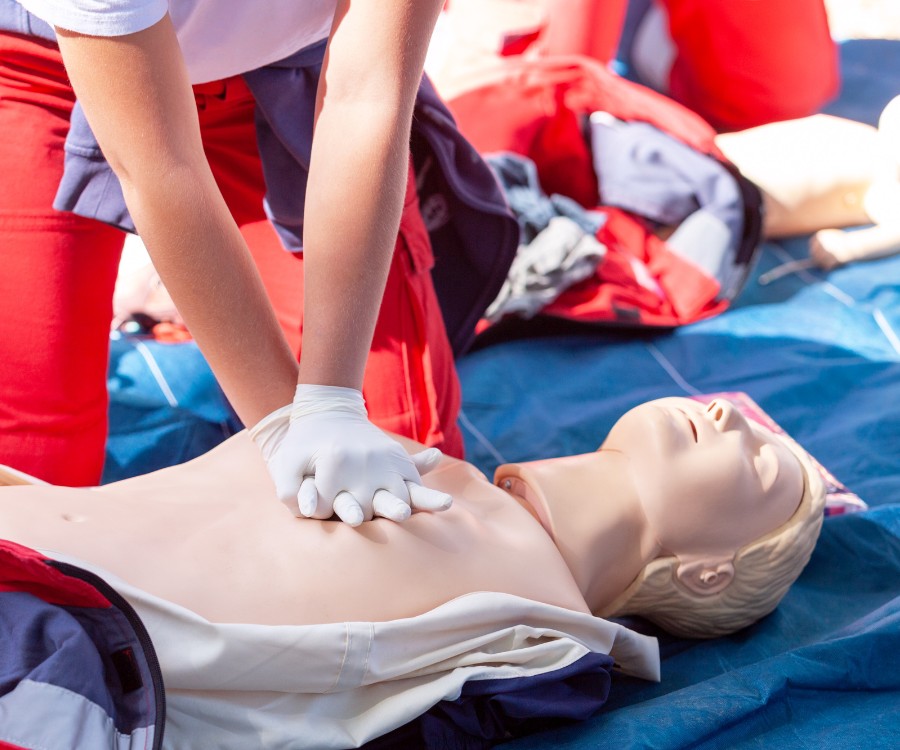
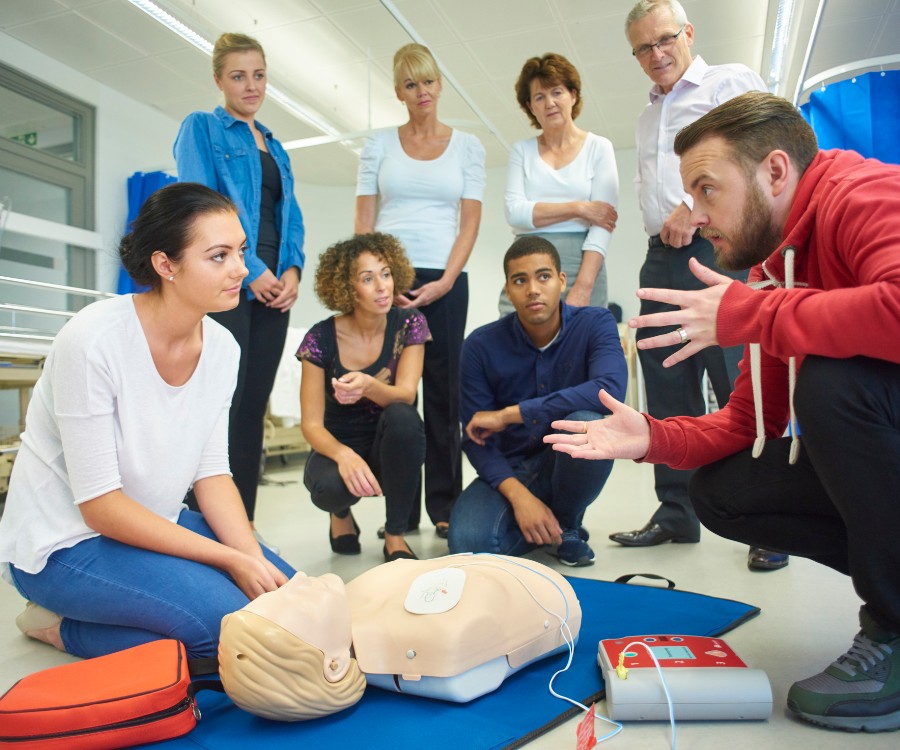
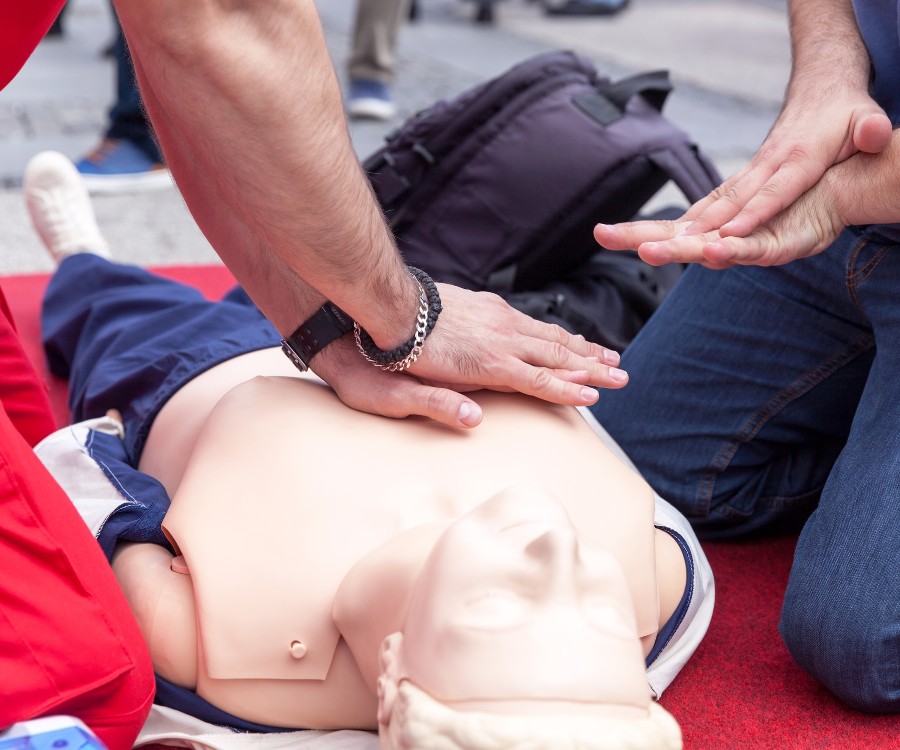
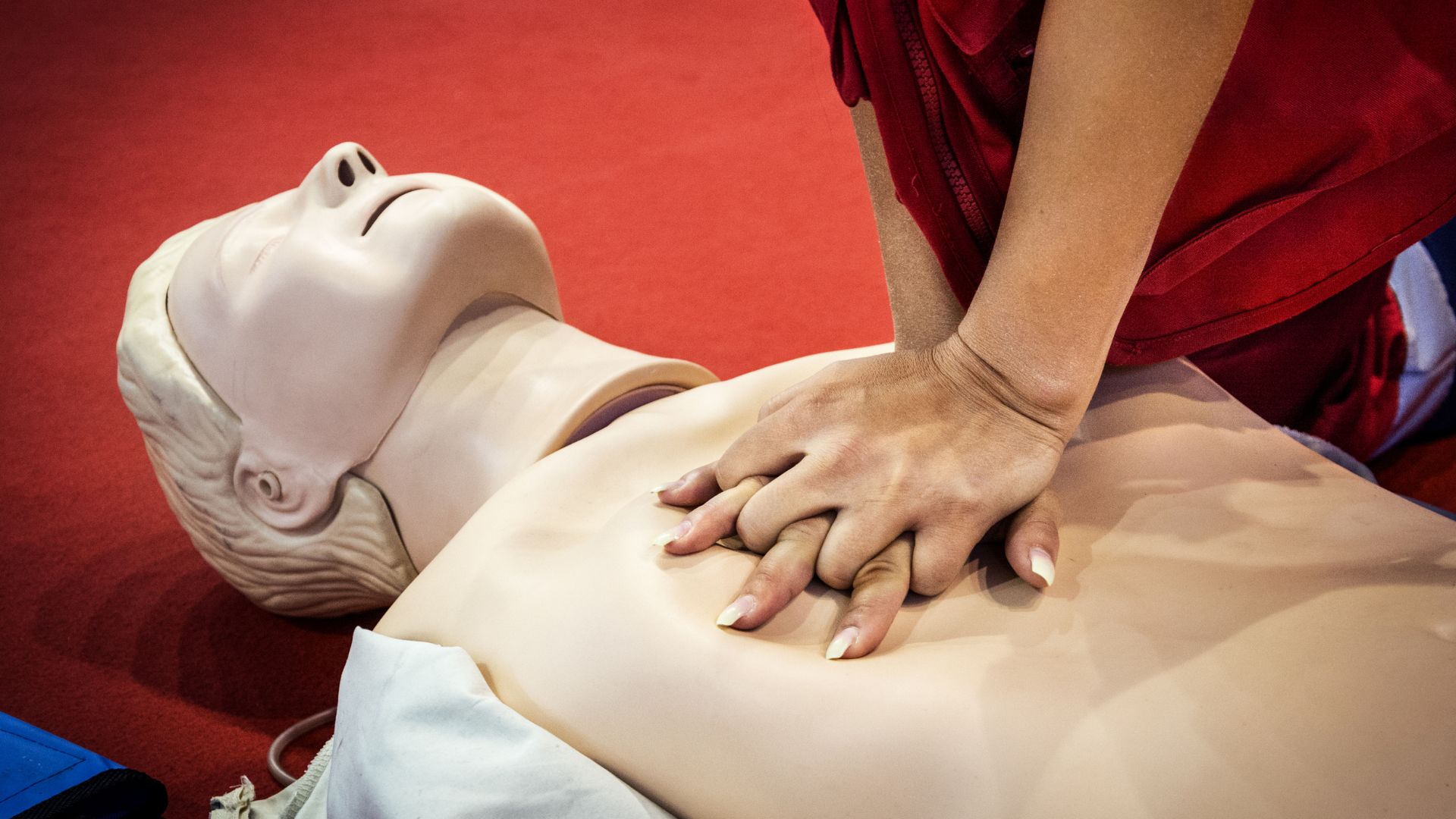
Why the Fears of Giving CPR Are Unfounded
People may fear giving CPR for one or more reasons. However, their explanations also clearly contradict the benefits of taking an on-site course and having this skill, especially if you’re a bystander.
The Reasons People Often Give for Not Taking CPR Classes
Lack of time – While people feel the time commitment is significant, you can schedule CPR classes on-site through In-Pulse CPR for a 3-hour session or for 5 hours if first Aad is included in the course.
Ask yourself how much time you normally take to go out to eat or to a ballgame? In most cases, CPR training takes less time.
You’ll learn a new skill and may save someone’s life as well. So, time really isn’t an issue. It’s just an excuse.
Not seeing themselves encountering situations where they’d use it – Some people feel they are unlikely to ever be in a situation where someone will need CPR. Therefore, they don’t see the value in spending the time or money to get trained.
However, emergencies can happen anytime, anywhere and to just about anyone. Wouldn’t you feel awful if you encountered an emergency tomorrow and you could have gotten certified but brushed it aside? You didn’t have the training that could possibly have saved someone’s life.
Not wanting the responsibility – Performing CPR, especially on a stranger, can no doubt be stressful. However, feeling helpless is even worse..
Unfortunately, some people worry about performing CPR correctly or about the potential legal implications if the victim doesn’t survive. This deters them from getting trained.
It’s important to note that Good Samaritan laws protect the bystander who is CPR trained. The medical help you can provide then far outweighs any legal implications, if any, that you’ll ever have to face.
In fact, you can get into more trouble if you don’t administer aid than if you go ahead and provide the necessary emergency care.
For example, in Minnesota, not giving medical assistance is considered a misdemeanor offense. Also, in Florida, the Good Samaritan Act (Florida Statute 768.13) includes a clause that protects people who use an automated external defibrillator (AED) during an emergency.
Even uncertified CPR is usually legal and may be performed in an emergency. However, you should still receive on-site CPR certification to improve the outcome in emergencies.
Also, it’s helpful to remember that 9-1-1 dispatchers can also guide you through CPR if you’re feeling nervous and need backup support at the scene.
The expense of a basic life support (BLS) course – A course in BLS costs around $55 (per In-Pulse). This amount is the same as what you’d pay for treating a family of four to dinner or for two or three refills of gas at the pump.
You can also get a haircut for this price or pay the same amount for a sporting event or admission into an amusement park. You might also pay the same amount for a video game or a good bottle of wine.
While not completely insignificant, this amount is comparable to many regular everyday purchases. Yet, learning a life-saving technique like CPR has a much more long-term value than the many everyday luxuries we enjoy and seemingly afford without a thought. Gaining emergency response skills truly is priceless for both ourselves and the loved ones around us.
The minimal investment you make is well worth safeguarding another person’s health and well-being. After all, the same people you may be protecting are also the ones you spend time with at amusement parks, restaurants, and sporting-related activities.
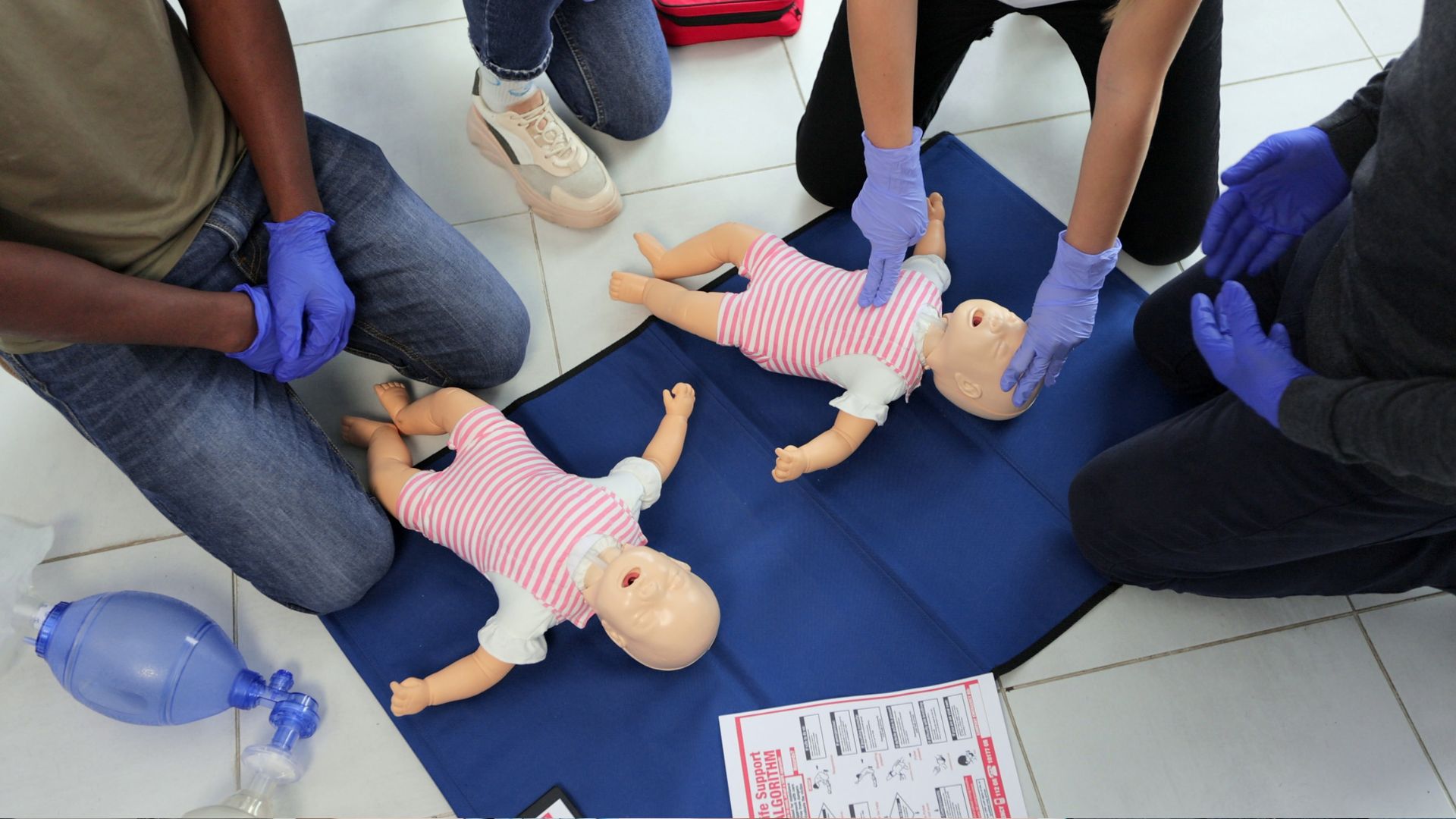
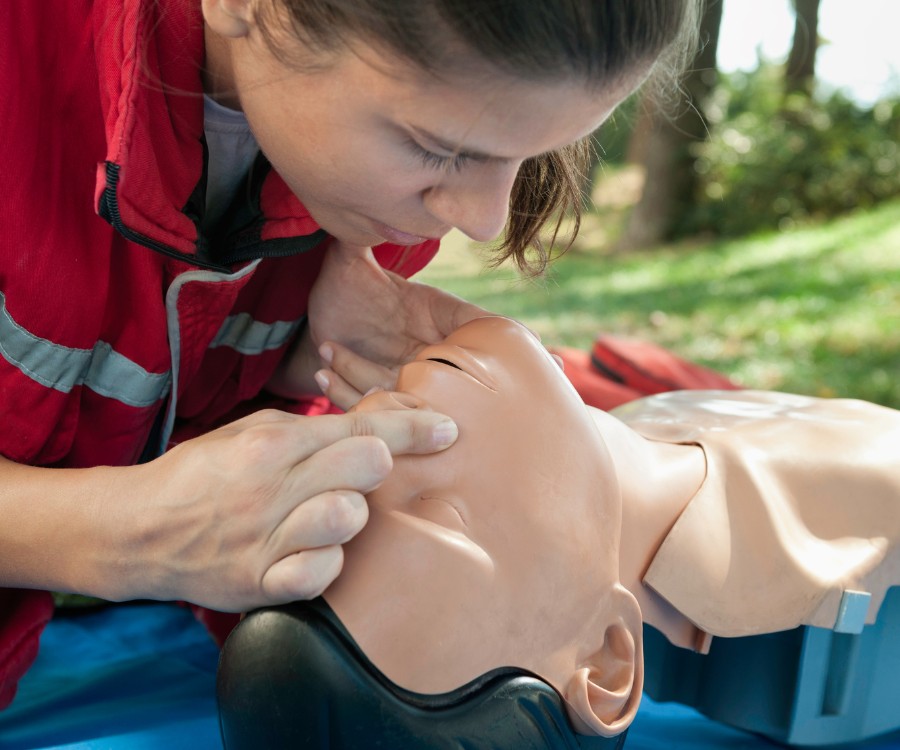
Discomfort with giving mouth-to-mouth resuscitation – Besides giving rescue breaths, untrainted responders can also learn how to save lives by learning hands-only CPR. This training, along with learning how to use an AED, still can be done without giving mouth-to-mouth.
Fear of infection – Some people, especially since the COVID pandemic, worry about infections. However, the use of barriers or masks can significantly reduce an infection risk while notably increasing the percentage of people who are saved.
Out-of-Hospital Cardiac Emergencies: Some Key Facts to Consider
When you consider the facts about out-of-hospital CPR emergencies, it does not make sense why anyone would not choose to take a BLS rescue course. For example, consider the following statistics:
- More than 350,000 cardiac arrests take place outside of U.S. hospitals each year. That averages to around 1,000 people per day experiencing a sudden cardiac arrest or SCA.
- As many as 70% of out-of-hospital cardiac arrests occur in home or private settings, with the remainder taking place in a public venue.
- Only about 10% of people survive an out-of-hospital cardiac arrest in the U.S. However, if a bystander has been CPR trained, the survival rate doubles or even triples, thereby making bystander CPR an urgent skill to have.
Make It Your New Year’s Resolution to Learn On-Site CPR through In-Pulse this year
Do you want to make a good start in the coming year? If so, why not make it your New Year’s Resolution to learn CPR? There’s an In-Pulse class waiting for you to attend! Sign up now and make this year your best year yet!