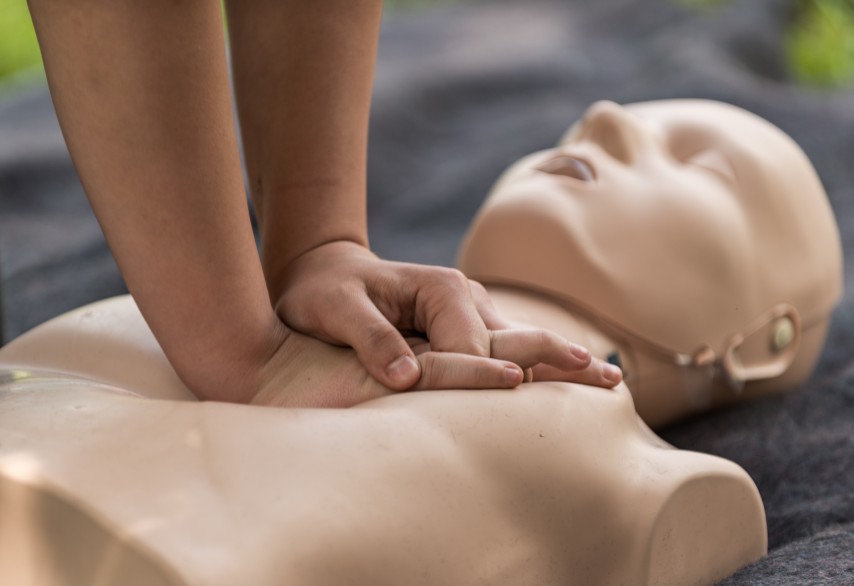
How to Get Your AHA BLS Renewal in the Twin Cities: A 2026 Guide for MN Nurses and Healthcare Pros
If your BLS card is close to expiring, this is not the time to take chances on a course that sounds convenient but could create problems later. In Minnesota, nursing renewal comes with continuing education and documentation requirements, and many employers, schools, and clinical sites across the Twin Cities expect current, instructor-led credentials. If you need to find a class quickly, you can view upcoming AHA BLS classes in Minnesota here.
For many nurses, CNAs, and medical assistants, the issue is pretty simple. You need the right BLS card, from a provider employers recognize, without burning your day off on online modules, tech issues, or multiple appointments.
Does the Minnesota Board of Nursing Accept Online-Only CPR?
The Minnesota Board of Nursing requires 24 contact hours of continuing education for RNs and 12 for LPNs every two years. While the Board does not endorse one single CPR provider, many major Twin Cities health systems, including Allina Health, M Health Fairview, and Mayo Clinic, commonly expect Healthcare Provider level BLS with a hands-on skills check.
That is where people can get tripped up. Some fast online-only courses look legitimate at first, but if there is no real instructor involvement or hands-on evaluation, the card may not be accepted where you need it. For most healthcare professionals, the safer choice is an official AHA BLS Provider course with a certified instructor.
Full Classroom vs. Hybrid: Why In-Person Often Feels Easier
Some competitors, including SureFire CPR, promote a 24/7 model that uses self-guided kiosks and smart manikins. For some people that may sound convenient, but for many healthcare professionals it ends up feeling like one more thing to manage.
- No extra homework: SureFire requires a 2 to 4 hour online module before you can even do the skills portion. With In-Pulse CPR, there is no pre-work required. You show up, complete the class, and move on with your day.
- Real instruction matters: At a kiosk, you are mostly working through the process on your own. In a live class, you can ask questions, get corrected in real time, and learn from an instructor with actual field or clinical experience.
- Simpler scheduling: You are not dealing with entry codes, separate steps, or technical support. You register, attend class, and finish everything in one visit.
Where to Find BLS Classes in the Twin Cities and West Metro
Location matters more than people think, especially when you are trying to fit renewal around work, school, or family. While some competitors focus heavily on Edina or Roseville, we offer convenient access for healthcare professionals in the west metro, including Plymouth, Wayzata, Minnetonka, and Maple Grove, as well as those in Minneapolis, St. Paul, Bloomington, and Woodbury.
You can check our Minnesota CPR class schedule here to find a class that fits your shift or school schedule.
Top Metro Employers and Schools That Require AHA BLS
In Minnesota, an AHA BLS card is often seen as the standard for healthcare roles and clinical programs. It is commonly required for:
- Health systems: Allina Health, M Health Fairview, North Memorial, and Children’s Minnesota.
- Nursing and allied health students: Programs connected to the University of Minnesota, St. Catherine University, and MCTC often require documented BLS before clinical participation.
FAQs for Minnesota Healthcare Professionals
What if my Minnesota license or job deadline is at the end of the month?
That is one of the biggest reasons people look for a local class. We provide official AHA eCards the next day as class completion, so you can send documentation to HR or your program quickly.
Is Red Cross or AHA better for Twin Cities healthcare jobs?
Some employers accept either, but many hospitals, clinics, and surgery centers in Minnesota specifically ask for the AHA BLS Provider card. That is why many healthcare workers choose AHA from the start.
Do I have to complete anything before class?
Not with us. We keep it straightforward. The education, skills, and testing are handled in one session, with no logins, no module problems, and no extra homework ahead of time.
A Smarter Way to Renew in Minneapolis and St. Paul
If you are renewing in the Twin Cities, the best option is usually the one that is local, recognized, and easy to complete without extra hassle. A good class should help you get in, get trained, and get the documentation you need without turning it into a project.
License expiring soon? We stand behind the certifications we issue. Employer rejection is very rare, but if there is ever a problem with acceptance, we will make it right or provide a full refund. We have trained more than 150,000 students with a strong focus on employer-accepted, hands-on certification.
Register for your Twin Cities BLS renewal class here and get your official AHA eCard the next day.